 |
 |
- Search
| Neonatal Med > Volume 29(4); 2022 > Article |
|
Abstract
Lethal neonatal rigidity and multifocal seizure syndrome (RMFSL) is a severe autosomal recessive epileptic encephalopathy characterized by rigidity, intractable multifocal seizures, microcephaly, apnea, and bradycardia immediately after birth. RMFSL is related to a mutation in breast cancer 1-associated ataxia telangiectasia mutated activation-1 protein (BRAT1). We report a case of a female infant born to non-consanguineous Korean parents who developed hypertonia, dysmorphic features, progressive encephalopathy with refractory seizures at birth, and worsening intermittent apnea, leading to intubation and death at 137 days of age. The initial repeated electroencephalographic findings were normal; however, a pattern of focal seizures emerged at 35 days of life. Rapid trio whole-exome sequencing revealed heterozygous mutations c.1313_1314delAG p.(Gln438Argfs*51) and c.1276C>T p. (Gln426*) in BRAT1. After genetic counseling for pregnancy planning, a preimplantation genetic diagnosis for targeted BRAT1 mutations was successfully performed, and a healthy baby was born. To our knowledge, this is the first reported case of a Korean patient with compound heterozygous mutations in BRAT1. An early and accurate genetic diagnosis can help provide timely treatment to patients and indicate the need for reproductive counseling for parents for family planning.
Lethal neonatal rigidity and multifocal seizure syndrome (RMFSL, OMIM #614498) is a severe epileptic encephalopathy characterized by rigidity and multifocal intractable seizures, microcephaly, and apnea, as well as severe bradycardia that leads to cardiac arrest and death. This syndrome is caused by a mutation in the breast cancer 1-associated ataxia telangiectasia mutated activation-1 protein (BRAT1) gene [1,2]. There are a few reports of this syndrome in the literature, most of which were cases of infants born to consanguineous parents who died within a few months of their 1st year of life. Herein, we report the first Korean neonate who was diagnosed with compound heterozygous BRAT1 mutations and the successful application of preimplantation genetic diagnosis (PGD) for targeted BRAT1 mutations for the next pregnancy.
A female infant was born to non-consanguineous parents at 40 weeks plus 1 day of gestation. The findings of several intrauterine ultrasound examinations performed during pregnancy were normal. The patient was delivered via emergency cesarean section because of failure to progress in labor. The Apgar scores were 8 and 9 at 1 and 5 minutes, respectively. Her birth weight was 3,310 g (40th percentile, ŌĆō0.26 standard deviation [SD]), her length was 49 cm (25th percentile, ŌĆō0.69 SD), and her head circumference was 32.5 cm (5th percentile, ŌĆō1.65 SD). Shortly after birth, the patient was noted to have frequent myoclonic seizure-like activity with hypertonia. Microcephaly with a small anterior fontanelle, clubfoot, low-set ears, and small forehead was observed at birth. The patient was subsequently transferred to a tertiary hospital for further evaluation. On admission to the neonatal intensive care unit, the patient was markedly hypertonic with contractions of the elbows and wrists and scissoring of both lower limbs. Neonatal reflexes were not elicited because of the increased muscle tone. Myoclonic jerks were prominent in the extremities and face in response to touch.
Electroencephalography (EEG) and brain magnetic resonance imaging (MRI) were performed on the 1st day of life. The EEG results were unremarkable. However, brain MRI revealed a diffusely decreased cerebral volume with a markedly prominent subarachnoid space and operculum widening with normal myelination. There were no abnormal signal changes in either the basal ganglia or the thalami (Figure 1A-D). Toxoplasmosis, rubella, cytomegalovirus, herpes simplex, and other septic workup were all negative, and findings on comprehensive neurometabolic tests such as neonatal screening test, amino acid, lactate, ammonia, acylcarnitine profile, urinary ketones, and quantitative amino acid and organic acids in urine did not reveal any abnormalities.
Hypertonia with rigidity and myoclonic seizure-like activities worsened, and the patient was eventually intubated at 25 days of age because of frequent apnea, bradycardia, and desaturation. Phenobarbital and levetiracetam were inefficacious, baclofen and clonazepam were added to treat hyperekplexia. Serial routine EEGs revealed normal results during the 1st month of life. At 35 days of age, we observed frequent clinical seizures with ictal activity from video-EEG monitoring. Serial video-EEG follow-ups revealed multifocal medium-to-high-voltage sharp wave discharges, predominantly on the left of the right central regions (Figure 2). As the patient did not respond to antiepileptic drugs, including phenobarbital, levetiracetam, baclofen, clonazepam, valproate, and vitamin challenges, a continuous infusion of midazolam was administered at approximately 43 days of life. Although midazolam was partially effective, the seizures were not completely controlled. We performed chromosomal microarray and rapid trio whole-exome sequencing for decision making regarding early onset intractable myoclonic seizures, hypertonia, and microcephaly. Serial brain MRI at 65 days of age revealed suspicious cystic encephalomalacia changes in bilateral parietal areas and interval-progressed atrophic changes in the cerebellum and brainstem (Figure 1E-H).
During the admission period, the patientŌĆÖs weight and length remained within the normal range, while her head circumference decreased below the 3rd percentile (Figure 3). The patient had feeding problems necessitating a nasogastric tube owing to poor oral sucking and recurrent aspiration.
At 89 days of age, rapid trio whole-exome sequencing revealed a heterozygous mutation in the BRAT1 gene, c.1313_1314delAG p.(Gln438Argfs*51) and c.1276C>T p.(Gln426*) (NM_152743.4), which were subsequently validated by Sanger sequencing (Figure 4). This mutation has previously been reported in the literature and is regarded as pathogenic. The patient died 137 days after birth. An autopsy was not performed according to the parentsŌĆÖ requests. For subsequent planning of pregnancy, we recommended PGD for the BRAT1 gene. Only unaffected embryos were transferred, and singleton pregnancy was achieved. At 12 weeks, chorionic villus sampling was performed for re-confirmation of the genotype of transferred embryos, and an unaffected fetus was confirmed by the polymerase chain reaction method. Consequently, a healthy girl was born.
RMFSL is a severe epileptic encephalopathy caused by BRAT1 gene mutations [1]. BRAT1 encodes a protein that interacts with tumor suppressor breast cancer gene 1 (BRCA1) and binds to ataxia telangiectasia mutated 1 gene (ATM-1) [2]. It is involved in cell cycle signaling pathways required for cellular responses to DNA damage [2]. The neuropathological examination has been reported in five cases, showing progressive atrophy and neuronal cell loss in the cerebrum and cerebellum, suggesting that disturbed apoptosis may occur because of BRAT1 mutations [3,4]. Several recent studies have demonstrated that loss of BRAT1 inhibits growth signaling, increases apoptosis, and induces mitochondrial dysfunction, which is involved in mitochondria-dependent intrinsic apoptosis [5].
The clinical features of RMFSL include progressive encephalopathy with hypertonia and hyperreflexia, microcephaly, various dysmorphic features, and developmental delay. After Puffenberger et al. [1] first reported three Amish infant siblings homozygous for the BRAT1 frameshift mutation (c.638_639insA) in 2012, an additional 24 severe cases of the spectrum (a total of 27) have been reported. Patients with the severe type are described and compared to our case in Table 1 [1,3,4,6-18]. A severe phenotype of RMFSL characterized by prenatal or neonatal onset of refractory myoclonic seizures, episodes of apnea, and absence of developmental progression leads to death within weeks to months of birth [3]. All EEGs were previously reported to be abnormal at the time of the evaluation. EEG typically shows diffuse slowing, consistent with encephalopathy, and (multi)focal sharp wave activity, consistent with ictal activity. Most brain MRI results were normal at the initial evaluation and demonstrated variable degrees of cerebral and/or cerebellar atrophy in serial follow-ups [4,14,15,17]. In our case, the clinical presentation was similar to that of other severe phenotypes. MRI findings showed significant cerebral atrophy on the 1st day of life, potentially indicating the sequelae of chronic exposure to refractory seizures during the prenatal period. However, serial routine EEGs during the 1st month of life did not reveal any abnormalities. Since the EEG findings were not pathognomonic during the 1st month and there were no other structural, metabolic, or infectious causes, we initially considered the symptoms presented in this case to represent hyperekplexia. However, the patientŌĆÖs hypertonia with rigidity and refractory myoclonic seizures worsened, and invasive ventilator support was required for frequent apnea, bradycardia, and desaturation. Epilepsy of a genetic origin, such as RMFSL, was suspected. Because BRAT1 was not included in the neonatal-onset genetic epilepsy panel, we performed rapid trio whole-exome sequencing for decision-making at 35 days of life, and the results were obtained at 54 days.
The importance of genetic testing has recently been emphasized. New genes responsible for neonatal-onset epilepsy have been rapidly discovered, and BRAT1 has been shown to cause RMFSL [16,17]. Shellhaas et al. [19] reported that more than three-quarters of the neonates with epileptic encephalopathies were genetically confirmed. Because many neonatal epilepsy syndromes have a genetic etiology, genetic testing should be considered as soon as possible to provide targeted treatments [19]. In addition, for the next pregnancy, genetic counseling of the parents should be considered. PGD can provide an alternative to prenatal diagnosis and selective abortion for parents at risk of transmitting a serious genetic disorder. Oocytes or cleaving embryos obtained from in vitro fertilization and biopsied cells were used for genetic diagnosis. Only embryos identified as free of genetic disorders were transferred into the uterus [20].
In our case, the patient presented with a severe RMFSL phenotype and was determined to have a heterozygous nonsense or frameshift mutation in the BRAT1 gene. PGD was successfully applied to the next pregnancy, and a healthy baby was born. To our knowledge, this is the first reported case of successful PGD for BRAT1 mutations in Korea.
In conclusion, genetic studies can be helpful for patients with severe epileptic encephalopathy. This report highlights the role of rapid trio whole-exome sequencing in early diagnosis and genetic counseling. Early and accurate genetic diagnosis can provide timely management to patients and indicate the need for reproductive counseling for parents for planning the next baby.
ARTICLE INFORMATION
Ethical statement
This study was approved by the Institutional Review Board of Seoul National University Bundang Hospital (IRB approval number: B-2206-763-701), and written informed consent was obtained from the patientŌĆÖs parents. The patientŌĆÖ parents provided informed consents for the publication of the present report.
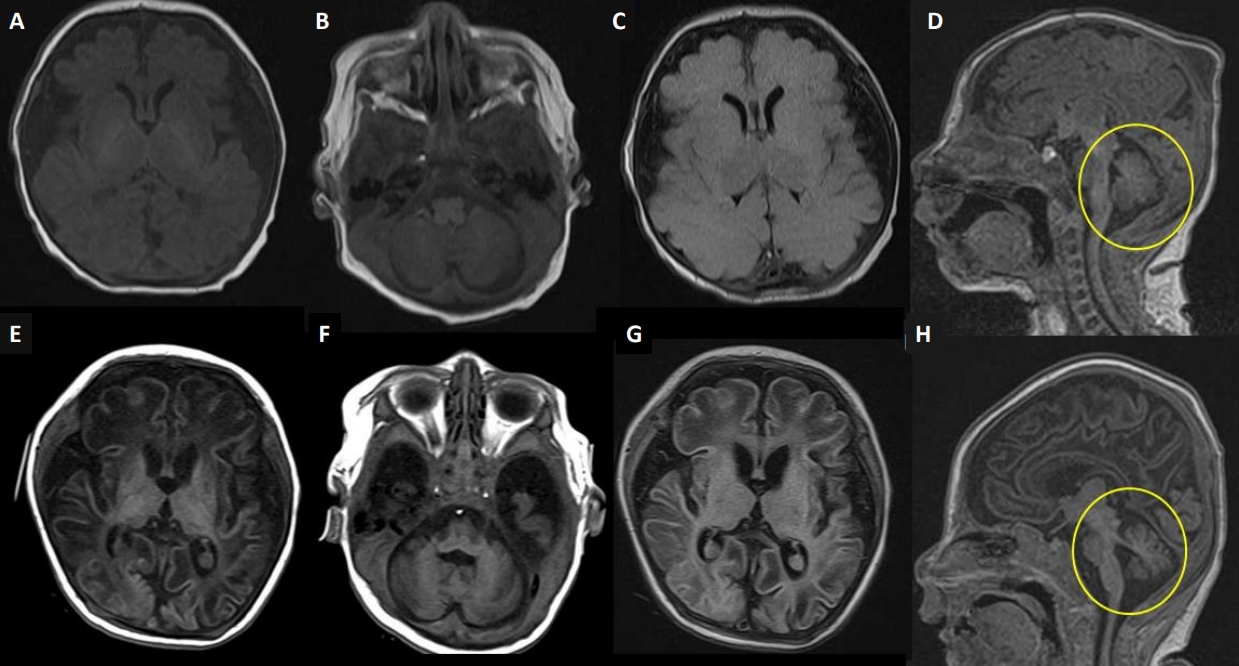
Figure┬Ā1.
Brain magnetic resonance imaging (MRI) scans. Upper row at day 1 of life (A-D), lower row at 2 months (E, F). (A, B, E, F) Axial T1-weighted images; (C, G) axial T2-weighted axial fluid-attenuated inversion recovery (FLAIR) images; and (D, H) sagittal T1-weighted images. (A-D) Brain MRI on day 1 showed a diffusely decreased volume of the cerebrum with a markedly prominent subarachnoid space and operculum widening with normal myelination. However, there were no demonstrable abnormal signal changes in the basal ganglia or the thalami. (E-H) Brain MRI at 2 months showed suspicious cystic encephalomalacia changes in bilateral parietal areas and progressive atrophy of the cerebrum, cerebellum, and brainstem (circles on E, F).
Figure┬Ā2.
Electroencephalography (EEG) findings. Ictal EEG at 35 days showing repetitive medium-to-high-voltage sharp wave discharges (arrows) from the right central region to the right hemisphere.

Figure┬Ā3.
Growth curves of the patient. (A) Growth curves showing the patientŌĆÖs body weight and length. (B) Growth curve showing the patientŌĆÖs head circumference.

Figure┬Ā4.
Pedigree and Sanger sequencing. Pedigree of the family. Wild-type alleles are indicated using +. A compound heterozygous mutation in breast cancer 1-associated ataxia telangiectasia mutated activation-1 protein (BRAT1) validated by Sanger sequencing. The frameshift mutation (c.1313_1314delAG) was found in the father and the patient, and the nonsense mutation (c.1276C> T) was confirmed in the mother and the patient.

Table┬Ā1.
Characteristics of 27 Previously Reported Cases with Severe Clinical Form of BRAT1-Related Rigidity and Multifocal Seizure Syndrome
| Study | Gender/Cons | Origin | BRAT1 mutation |
Micr |
Hypertonia | Seizure onset | Seizure type | EEG pattern (timing of examination) | Initial MRI (timing of examination) | Age at death | |
|---|---|---|---|---|---|---|---|---|---|---|---|
| At birth | Prog. | ||||||||||
| Puffenberger et al. (2012) [1] (family, n=3) | NK | Amish | Homozygous c.638_639 insA, p.(Val214Glyfs* 189) | + | + | + | Soon after birth | Focal jerks of the tongue, face, and arms | Bilateral medium-high voltage spikes over the temporal and central regions, frequent multifocal seizures, background slowing, and no posterior rhythm (NK) | Normal or mild hypoplasia of the frontal lobes (NK) | <4 mo |
| Saunders et al. (2012) [18] (n=1) | F/+ | Mexican | Homozygous c.453_454 insATCTT CTC, p.(Leu1 52Il efs *70) | + | NK | + | Soon after birth | NA | Focal epileptiform and sharp wave activity (1 d) | Normal (1 d) | NK |
| Saitsu et al. (2014) [4] (family, n=2) | F/ŌĆō | Japanese | Compound Heterozygous c.176T>C, p.(Leu59Pro); c.962_963del ,p.(Leu321 Profs*81) | ŌĆō | + | + | 7 d | Generalized tonicclonic and myoclonic seizures of the limbs and face | Generalized tonic┬Łclonic and myo┬Ł clonic seizures of the limbs and face | Progressive cerebral and cerebellar atrophy (4 mo) | 1 yr 9 mo |
| F/ŌĆō | ŌĆō | + | + | 1 d | Myoclonic, clonic, and tonic seizures | Myoclonic, clonic, and tonic sei┬Ł zures | Mild cerebral, cerebellar atrophy, and delayed myelination (3 mo) | 3 mo | |||
| Straussberg et al. (2015) [17] (family, n=2) | F/+ | Arabic | Homozygous c.1173delG, p.(Leu391fs) | NK | + | + | 1 d | Myoclonic | Sharp waves and bilateral spikes predominantly over the right he┬Ł misphere (NK) | Normal (NK) | 5 mo |
| M/+ | ŌĆō | ŌĆō | + | 1 d | Myoclonic | Bilateral epileptic activity with bilateral discharges (NK) | Normal (NK) | 6 mo | |||
| van de Pol et al. (2015) [16] (family, n=3) | M/+ | Moroccan | Homozygous c.638dup, p. (Val214Glyfs*189) | ŌĆō | ŌĆō | + | 1 mo | Tonic, clonic | Severely abnormal background pattern with multifocal sharp waves, and frequent multifocal epileptic seizure activity (NK) | Rather small cerebellum and brainstem (7 wk) | 3.5 mo |
| F/+ | ŌĆō | + | + | 1 mo | Eye blinking, myoclonus of the left hand | Continuous abnormal backgro┬Ł und pattern, multifocal activity (NK) | Normal (2 mo) | 17 mo | |||
| M/+ | ŌĆō | + | + | 1 mo | Tonic, myoclonic | Burst┬Łsuppression pattern with long suppressions (10ŌĆō15 sec), multifocal negative sharp waves (6 wk) | NA | 2 mo | |||
| Horn et al. (2016) [15] (n=1) | M/ŌĆō | German | Compound heterozygous c.638_639insA, p.(Val214 Glyfs*189) c.1134+1G>A | ŌĆō | + | + | 1 d | Myoclonic | Diffuse slowing, bilateral spikes, and partly a burst┬Łsuppression pattern, epilepsia partialis con┬Łtinua (NK) | Normal (NK) | 2 mo |
| Smith et al. (2016) [14] (n=1) | M/ŌĆō | NA | Compound heterozygous c.1857G>A; p.(Trp619*); c.2125_2128delTTTG, p.(Phe709Thrfs*17) | ŌĆō | + | + | 4 mo | Facial myoclonus, focal dyscongnitive, and secondarily generalized seizures | Bilateral multifocal epileptiform activity with frequent clinical and electrographic seizures (NK) | Normal (2 mo) | 15 mo |
| Celik et al. (2017) [13] (n=1) | M/+ | Turkish | Homozygous c.2230_2237 dupAACACTGC, p.(Ser 747Thrfs*36) | ŌĆō | + | + | NK | Myoclonic seizures of the limbs and face | Background activity of 4ŌĆō6 Hz theta, bilateral frontotemporal sharp waves, and 8ŌĆō10 Hz ictal rhythm during clinical seizures (27 d) | Normal (soon after birth) | 10 mo |
| Hegde et al. (2017) [12] (n=1) | F/+ | Indian/Muslim | Homozygous c.617T >A, p. (Leu206*) | NK | + | + | 3 d | Clonic seizures, eye blinks, and mouth movements, migrating partial epilepsy of infancy | Clinical and subclinical seizures with migrating variable focus over both hemispheres (56 d) | Mild ventriculomegaly with prominent subarachnoid spaces (7 d) | 4 mo |
| Szymanska et al. (2018) [10] (family, n=2) | F/ŌĆō | NK | Homozygous c.1313_131 4delAG, p.(Gln438fs) | NA | NA | + | 1 d | Myoclonic | NA | Brain atrophy with a pro┬Ł nounced white matter vol┬Ł ume loss, thinning of the corpus callosum (5 mo) | 6 mo |
| M/ŌĆō | NK | + | + | 1 d | Myoclonus, clonic and tonic seizures | Generalized and focal sharp and spike waves (NK) | Widened subarachnoid space (2 wk) | 12 mo | |||
| Van Ommeren et al. (2018) [3] (n=1) | F/ŌĆō | Chinese | Homozygous c.1395G>C, p.(Thr465Thr) | NA | + | + | 1 d | Myoclonic | Diffuse encephalopathy, with fre┬Ł quent ictal activity from multiple cortical areas (1 d) | Small head, small brain, and mild prominence of pericerebral extraaxial space (3 d) | 10 wk |
| Colak et al. (2020) [9] (n=1) | M/+ | Turkish | Homozygous c.1499-1G>T | ŌĆō | + | ŌĆō | 1 d | Myoclonic | Generalized epileptiform activity, migrating focal epileptiform ac┬Ł tivity (2 mo) | Atrophic corpus callosum, hypomyelination, cortical laminar necrosis in both occipital and superior parietal lobes, brainstem and cerebellar vermis hy┬Ł poplasia (NK) | 7.5 mo |
| Scheffer et al. (2020) [8] (family no. 4, n=5) | F/ŌĆō | Fillipino/Irish | Compound heterozygous c.964C>T, p.(Gln322*); c.2284C>T, p.(Gln762*) | + | + | + | 1 d | Focal motor seizures, migrating between hemispheres | Multifocal epileptiform discharges, migrating focal seizures (NK) | Asymmetric T2 signal in deep posterior parietal white matter bilaterally likely due to white matter oedema (3 d) | 34 d |
| F/ŌĆō | + | + | + | 1 d | Focal clonic seizures migrating between hemispheres | Multifocal epileptiform discharges, migrating focal seizures (NK) | Mild thinning of corpus callosum (2 d) | 10 mo | |||
| F/+ | Pakistani | Homozygous c.1498+1G>A | + | + | + | 1 d | Focal, multifocal motor seizures with clonic features, often epileptic spasms; tonic seizures | Multifocal epileptiform discharges, migrating focal seizures, epileptic spasms and periodic spasms, hypsarrhythmia (NK) | Very small hemosiderin deposition within lateral ventricles (1 mo) | 4 yr 3 mo | |
| M/+ | Caucasian | Homozygous: c.1120G>T, p.(Glu374*) | ŌĆō | + | + | 4 d | Myoclonic, focal clonic seizures | Multifocal epileptiform discharges, myoclonic seizures; focal clonic seizures migrating between he┬Ł mispheres (NK) | Small subacute subdural hemorrhage along tento┬Ł rium with left parietal bone cephalhematoma (17 d) | 2 mo | |
| F/ŌĆō | Chinese | Compound heterozygous c.1359_1361delCCT,p.(Leu454del);c.1395G>C, p.(Thr465Thr) | + | + | + | Soon after birth | Myoclonic, migrating focal clonic seizures | Multifocal epileptiform discharges, migrating focal seizures (NK) | Small right occipital sub┬Ł dural hemorrhage (3 d) | 14 mo | |
| Li et al. (2022) [7] (n=1) | F/ŌĆō | Chinese | Homozygous c.233G >C, p.(Arg78Pro) | ŌĆō | + | + | 1 mo | Myoclonic | Focal sharp wave discharges and spike and slow wave complex in the forehead┬Łtemporal region (NK) | Widened bilateral frontal and temporal subarach┬Ł noid space (NK) | 7 mo |
| Pourahmadi┬Ł yan et al. (2021) [6] (n=1) | M/NK | Iranian | Homozygous c.2041G> T, p.(E681*) | + | NA | + | Soon after birth | Focal seizure | NA | NA | 6 d |
| Present case (n=1) | F/ŌĆō | Korean | Heterozygous c.1276C>T p.(Gln426*);c.1313_1314 delAG, p.(Gln438Argfs*51) | ŌĆō | Prog. Micr | + | Soon after birth | Generalized spasticity with hypertonia, refractory focal seizures | Normal (1 d), repetitive medium┬Ł to┬Łhigh voltage sharp wave dis┬Ł charges from right central region evolving to the right hemisphere (35 d) | Diffusely decreased volu┬Ł me of the cerebrum with markedly prominent subarachnoid space and operculum widening with normal myelination (1 d) | 4 mo |
Reproduced from Colak et al. [9], with permission from Springer Nature.
Abbreviations: BRAT1, breast cancer 1-associated ataxia telangiectasia mutated activation-1 protein; Cons, consanguinity; Micr, microcephaly; EEG, electroencephalogram; MRI, magnetic resonance imaging; NK, not known; NA, not assessed; Prog, progressive.
REFERENCES
1. Puffenberger EG, Jinks RN, Sougnez C, Cibulskis K, Willert RA, Achilly NP, et al. Genetic mapping and exome sequencing identify variants associated with five novel diseases. PLoS One 2012;7:e28936.



2. Aglipay JA, Martin SA, Tawara H, Lee SW, Ouchi T. ATM activation by ionizing radiation requires BRCA1-associated BAAT1. J Biol Chem 2006;281:9710ŌĆō8.


3. Van Ommeren RH, Gao AF, Blaser SI, Chitayat DA, Hazrati LN. BRAT1 mutation: the first reported case of Chinese origin and review of the literature. J Neuropathol Exp Neurol 2018;77:10718.
4. Saitsu H, Yamashita S, Tanaka Y, Tsurusaki Y, Nakashima M, Miyake N, et al. Compound heterozygous BRAT1 mutations cause familial Ohtahara syndrome with hypertonia and microcephaly. J Hum Genet 2014;59:687ŌĆō90.



5. So EY, Ouchi T. BRAT1 deficiency causes increased glucose metabolism and mitochondrial malfunction. BMC Cancer 2014;14:548.




6. Pourahmadiyan A, Heidari M, Shojaaldini Ardakani H, Noorian S, Savad S. A novel pathogenic variant of BRAT1 gene causes rigidity and multifocal seizure syndrome, lethal neonatal. Int J Neurosci 2021;131:875ŌĆō8.


7. Li W, Wu S, Xu H, Zhao X, Pan Y, Huang H, et al. Novel variant in BRAT1 with the lethal neonatal rigidity and multifocal seizure syndrome. Pediatr Res 2022;91:565ŌĆō71.



8. Scheffer IE, Boysen KE, Schneider AL, Myers CT, Mehaffey MG, Rochtus AM, et al. BRAT1 encephalopathy: a recessive cause of epilepsy of infancy with migrating focal seizures. Dev Med Child Neurol 2020;62:1096ŌĆō9.



9. Colak FK, Guleray N, Azapagasi E, Yazici MU, Aksoy E, Ceylan N. An intronic variant in BRAT1 creates a cryptic splice site, causing epileptic encephalopathy without prominent rigidity. Acta Neurol Belg 2020;120:1425ŌĆō32.




10. Szymanska K, Laure-Kamionowska M, Szczaluba K, Koppolu A, Furmanek M, Kusmierska K, et al. Clinico-pathological correlation in case of BRAT1 mutation. Folia Neuropathol 2018;56:36271.
11. Skafi O, Fawaz A, Merhi B, Jouni H, Mansour S, Harb R, et al. Rigidity with multifocal seizure syndrome, lethal neonatal in a Lebanese neonate. A rare case report. J Pediatr Disord Neonatal Care 2018;1:106.
12. Hegde AU, Sanghvi KP, Karnavat PK, Jalan AB. BRCA1-associated ataxia telangiectasia mutated activation-1 mutation: an addition to the early infantile epileptic encephalopathy panel. J Clin Neonatol 2017;6:200ŌĆō4.

13. Celik Y, Okuyaz C, Arslankoylu AE, Ceylaner S. Lethal neonatal rigidity and multifocal seizure syndrome with a new mutation in BRAT1. Epilepsy Behav Case Rep 2017;8:31ŌĆō2.



14. Smith NJ, Lipsett J, Dibbens LM, Heron SE. BRAT1-associated neurodegeneration: intra-familial phenotypic differences in siblings. Am J Med Genet A 2016;170:3033ŌĆō8.



15. Horn D, Weschke B, Knierim E, Fischer-Zirnsak B, Stenzel W, Schuelke M, et al. BRAT1 mutations are associated with infantile epileptic encephalopathy, mitochondrial dysfunction, and survival into childhood. Am J Med Genet A 2016;170:2274ŌĆō81.



16. van de Pol LA, Wolf NI, van Weissenbruch MM, Stam CJ, Weiss JM, Waisfisz Q, et al. Early-onset severe encephalopathy with epilepsy: the BRAT1 gene should be added to the list of causes. Neuropediatrics 2015;46:392ŌĆō400.


17. Straussberg R, Ganelin-Cohen E, Goldberg-Stern H, Tzur S, Behar DM, Smirin-Yosef P, et al. Lethal neonatal rigidity and multifocal seizure syndrome: report of another family with a BRAT1 mutation. Eur J Paediatr Neurol 2015;19:240ŌĆō2.


18. Saunders CJ, Miller NA, Soden SE, Dinwiddie DL, Noll A, Alnadi NA, et al. Rapid whole-genome sequencing for genetic disease diagnosis in neonatal intensive care units. Sci Transl Med 2012;4:154ra135.










