Neonatal Hemolytic Disease Caused by Anti-e and Anti-C Antibodies Treated with Intensive Phototherapy: A Case Report
Article information
Abstract
ABO and Rh incompatibility are the leading causes of hemolytic disease of the fetus and newborn (HFDN). Due to the high antigenicity of the D antigen, hemolysis and symptoms progress rapidly. However, minor blood group incompatibility manifests varying clinical symptoms, from asymptomatic cases to neonatal jaundice and fetal hydrops. This study presents a case of HFDN in which anti-C and anti-e antibodies were identified and treated with intensive phototherapy. A full-term infant weighing 3,100 g at birth, with no complications during delivery, presented with jaundice and was admitted for intensive phototherapy. Antibody testing detected anti-C and anti-e antibodies in the neonate and the mother. The patient responded well to phototherapy, and intravenous immunoglobulin was administered. The total bilirubin levels decreased, and the infant was discharged after 5 days. At the age of 12 months, the infant exhibited normal neurodevelopment. In conclusion, neonates with HFDN, due to rare minor blood incompatibility, specifically anti-C and anti-e antibodies, can mitigate hyperbilirubinemia using phototherapy. Future research should also consider the severity of the minor blood group incompatibility.
INTRODUCTION
Hemolytic disease of the fetus and newborn (HFDN), also known as alloimmune hemolytic disease in newborns, occurs in 3 to 80 per 100,000 newborns annually in the United States [1]. HFDN is mainly caused by the incompatibility of ABO and Rh blood groups. Among the different Rh blood types, RhD primarily causes hemolytic disease in newborns, whereas minor blood groups such as C, E, c, e, Kelly, and Duffy occur infrequently [2]. These minor group incompatibilities contribute to approximately 3% to 5% of neonatal hemolytic jaundice cases [3]. In a single-center study conducted in South Korea between 1999 and 2022, 18 cases of HFDN caused by minor Rh group incompatibility were identified in infants with unexpected antibodies, which included the identification of anti-M, anti-E & c, and anti-E antibodies [4]. Another single-center study reported HFDN in five patients between 2008 and 2015, involving three anti-E and two anti-E & c with unexpected antibodies [5]. Regarding HFDN caused by Rh incompatibility, the D antigen exhibits high antigenicity, leading to rapid hemolysis and symptoms progression. Conversely, minor blood group incompatibility leads to various clinical symptoms from asymptomatic condition to neonatal jaundice and fetal hydrops [6-8]. HFDN accompanied by anti-C and anti-e antibodies has been rarely reported, and no case has been reported in Korea yet.
In this study, we report a case of HFDN in which anti-C and anti-e antibodies were identified and the condition was successfully treated with intensive phototherapy. We reviewed the clinical characteristics of HFDN caused by anti-C and anti-e antibodies according to related studies.
CASE REPORT
The female newborn, delivered via cesarean section at 39 weeks and 3 days of gestation, had a birth weight of 3,100 g (41st percentile) and Apgar scores of 10 at 1 minute and 10 at 5 minutes. The mother had two previous births, two healthy surviving children, and no miscarriages. The mother had no maternal diseases throughout pregnancy, and the delivery was uneventful. The mother had blood type O- and was Rh-positive; unfortunately, the antibody screening test was not conducted during the prenatal examination at a local obstetric clinic. Before childbirth, the mother did not undergo any blood transfusions. Phototherapy was initiated on the 3rd day after birth due to jaundice. However, the transcutaneous total bilirubin level increased to 28.9 mg/dL, necessitating admission to the neonatal intensive care unit for treatment.
Upon admission, the neonate showed stable vital signs without seizures or specific high-pitched crying. Neurological examination revealed normal primitive reflexes, including the sucking and Moro reflexes, as well as normal muscle tone and tendon reflexes. There were no signs of delivery-related injury, heart murmur, or abdominal distension, and the umbilical cord was dry. Hemoglobin analysis showed normocytic normochromic anemia at a level of 9.4 g/dL. Electrolyte and C-reactive protein levels were within normal ranges. The neonate tested positive for blood types O and Rh; however, the direct Coombs test confirmed a positive result, suggesting the presence of antibodies. Further antibody testing revealed the presence of anti-e and anti-C antibodies in the neonate and the mother.
The patient underwent intensive phototherapy while preparing for a potential exchange transfusion following the established protocol [9]. After 3 hours of intensive phototherapy, the total bilirubin level decreased to 22.5 mg/dL, which was below the exchange transfusion threshold of 23 mg/dL for neonates aged 38 weeks or older with HFDN. Considering the patient's favorable response to phototherapy, intensive phototherapy was continued. Additionally, intravenous immunoglobulin (IVIg) was administered at a dose of 1 g/kg twice at a 12-hour interval. Subsequent assessments revealed declining total bilirubin levels of 21.4, 19.8, and 13.3 mg/dL at 9, 12, and 24 hours after intensive phototherapy, respectively. Magnetic resonance imaging indicated no bilirubin deposition in specific brain regions. Although there were no signs of convulsions, electroencephalography (EEG) revealed nonconvulsive seizures originating from the left occipital region, leading to the initiation of phenobarbital treatment. Five days after admission, the total bilirubin level decreased to 3.7 mg/dL, the hemoglobin level was 11.0 g/dL, jaundice symptoms improved, and the patient was discharged. Neonatal hearing screening yielded normal results. Subsequent EEG tests conducted 1 and 6 months after discharge were normal. Phenobarbital treatment was discontinued because the follow-up EEG showed normal activity 1 month later without convulsions. The EEG performed at 6 months was normal, and no neurological abnormalities were observed during physical examinations. By 12 months of age, the EEG test showed no seizures, and the outcomes of the K-Bayley III assessment were within the normal range.
DISCUSSION
Infants who presented symptoms of jaundice confirmed from the 3rd day of life were diagnosed with HFDN accompanied by anti-C and anti-e antibodies and recovered from hyperbilirubinemia through phototherapy. To date, a total of three cases of HFDN accompanied by anti-C and anti-e antibodies have been reported. In South Korea, two neonates have been identified in articles and abstracts; however, a case report has not been published yet.
In an Indian case, a preterm infant born at 35 weeks of gestation developed severe hyperbilirubinemia and jaundice 36 hours after birth and was effectively treated with intensive phototherapy [10]. A full-term Iranian newborn with anti-C & e antibodies presented with jaundice for 48 hours. Although the total bilirubin level rose to 17.1 mg/dL, the condition improved with phototherapy, and the newborn was discharged [11]. In a Korean case, a newborn with confirmed anti-C & e complex antibodies presented with neonatal jaundice on the 6th day after birth. The patient’s symptoms improved with phototherapy [12]. These neonates developed jaundice later than those with other antibodies, and their total bilirubin levels were not significantly high. Recovery from hyperbilirubinemia was possible with IVIg and intensive phototherapy without exchange transfusion. Exchange transfusion has only been conducted in Austria [13]. None of the patients exhibited neurological symptoms such as seizures or kernicterus (Table 1).
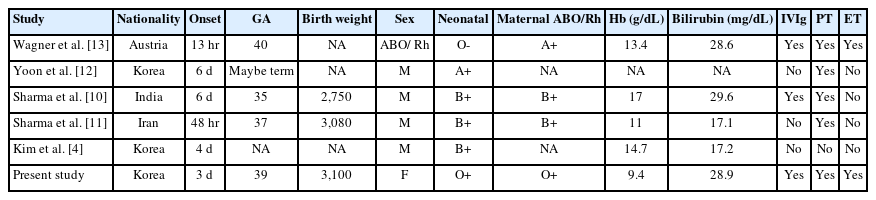
Clinical Characteristics of Five Cases of Hemolytic Disease of the Fetus and Newborn with Anti-C and Anti-e
The most severe outcome of neonatal jaundice is the development of kernicterus. Rapid elevation of indirect bilirubin levels can lead to the passage of free bilirubin through the blood-brain barrier, resulting in kernicterus. Exchange transfusion is recommended to prevent kernicterus neurotoxicity when hyperbilirubinemia does not respond to appropriate phototherapy or when caused by HFDN [9]. However, exchange transfusion is an invasive procedure carrying potential complications and a risk of death. Therefore, efforts to continue phototherapy with adjuvant treatments are made whenever possible. Based on findings from previously reported literature, jaundice induced by anti-C & e complex antibodies can be effectively treated with phototherapy, along with adjuvant therapy using IVIg, without requiring exchange transfusion.
HFDN caused by incompatibility of the main blood groups results in jaundice due to rapid elevation of bilirubin levels within 48 hours. However, considering the reported case of HFDN caused by anti-C and anti-e antibodies, such as in this patient, it predominantly occurred between the 3rd and 5th days. In this case, the bilirubin level at the first visit to the hospital was high enough to consider an exchange transfusion. However, since the patient did not exhibit any other symptoms, including neurological ones, only intensive phototherapy was administered, and the patient responded. Furthermore, due to clotting and blockage of the umbilical vein and artery within 48 hours after birth, cases of late-detected hyperbilirubinemia face challenges in locating suitable blood vessels for exchange transfusion.
In a single-center in South Korea, 2.45% of mothers tested positive for the antibody screening [14]. Although some skepticism exists about having all pregnant women tested for antibodies [15], antibody screening is recommended as a prenatal test for pregnant women to prevent neonatal hemolytic disease caused by unexpected antibodies [16]. However, in local obstetric clinics, it is often performed only when major blood group incompatibility is identified, similar to the case in the present study; routine antibody screening tests are often not performed. Had the antibody test been performed prenatally, treatment of the patient's symptoms could have been initiated earlier. A limitation of this study is the lack of Rh subtype testing. While the antibody test offered certain insights into antigen status, the diagnosis could have been improved, if possible, by identifying the specific Rh subtype.
In conclusion, through phototherapy, neonates with HFDN caused by rare minor blood incompatibility due to anti-C and anti-e antibodies could avoid hyperbilirubinemia, which is linked to kernicterus. Future research should also consider the severity of the minor blood group incompatibility.
Notes
Ethical statement
This study was conducted with the approval from the Institutional Review Board of Jeonbuk National University Hospital (No. 2023-06-039). This study was exempted from consent from the Institutional Review Board of Jeonbuk National University Hospital.
Conflicts of interest
Jin Kyu Kim is an editorial board member of the journal, but he was not involved in the peer reviewer selection, evaluation, or decision process of this article. No other potential conflicts of interest relevant to this article were reported.
Author contributions
Conception or design: G.J., H.H.K.
Acquisition, analysis, or interpretation of data: G.J., H.H.K.
Drafting the work or revising: G.J., J.K.K., S.J.K., H.H.K.
Final approval of the manuscript: All authors read and approved the final manuscript.
Funding
This research was supported by the Bio & Medical Technology Development Program of the National Research Foundation (NRF) funded by the Korean government (MSIT) (No. RS-2023-00236157).
Acknowledgements
None
