 |
 |
- Search
| Neonatal Med > Volume 27(1); 2020 > Article |
|
Abstract
Kaposiform hemangioendothelioma (KHE) is a rare, locally aggressive vascular neoplasm that often develops a coagulopathy known as Kasabach┬ŁMerritt phenomenon (KMP). Visceral involvement denotes a poor prognosis. We report a case of visceral KHE with KMP successfully treated with corticosteroids and vincristine. The infant had been born vaginally at 34 weeks 6 daysŌĆÖ gestation, weighing 2,360 g. He was admi tted for the management of respiratory failure. Blood tests showed anemia and thrombocytopenia 1 hour after delivery. Additional blood tests revealed a prothrombin time of 12.1 seconds, activated partial thromboplastin time of 60.6 seconds, fibrinogen levels of 72.4 mg/dL, and D┬Łdimer levels >3,200 ng/mL. Despite supportive measures and daily transfusions, the clinical condition and coagulopathy gradually worsened. Renal ultrasonography performed to find the origin of the coagulopathy revealed an echogenic mass measuring >3 cm in the abdominal cavity. A magnetic resonance imaging scan showed an ill┬Łmarginated, infiltrative mass like lesion in the right anteromedial and posteromedial perirenal space that was hypointense with mild enhance ment on T1┬Ł and T2┬Łweighted images. Large vascular tumors adherent to other visceral organs were noted during exploratory laparotomy but could not be resected. Treatment with methylprednisolone was ineffective. Vincristine was administered weekly from the 17th hospital day, and the coagulation profile showed gradual impro vement after its initiation. Intravenous methylprednisolone was switched to oral prednisolone on the 57th hospital day. He was discharged on the 73rd hospital day and continued vincristine treatment every 2 weeks and oral prednisolone administration as an outpatient treatment for 8 weeks. He remained symptom┬Łfree at the 39┬Łmonth follow┬Łup.
Kaposiform hemangioendothelioma (KHE) is a rare, locally aggressive vascular neoplasm with intermediate malignancy that often develops the Kasabach-Merritt phenomenon (KMP) [1]. It usually occurs in the soft tissues of infants, especially in the skin or retroperitoneum. Although visceral involvement is very uncommon, several cases with bone, retroperitoneal, or mediastinal involvement have been described [2]. KHE is accompanied by KMP in high frequencies, and those tumors complicated by KMP have poor prognoses [3]. Huge vascular tumors with KMP are accompanied by life-threatening clinical deterioration and associated with poor outcomes, particularly in newborns and infants. The optimal therapy for KHE with KMP has not been known thus far.
Here we report a neonatal case of visceral KHE with KMP successfully treated with corticosteroids and vincristine.
The infant had been born at our hospital to a 25-year-old woman (gravida 0, para 0) with preterm labor following an uncomplicated pregnancy and delivery. He was delivered vaginally at 34 weeks 6 daysŌĆÖ gestation. The Apgar scores were 6 at 1 minute and 8 at 5 minutes. He weighed 2,360 g.
He was admitted to the neonatal intensive care unit for the management of respiratory failure that included tachypnea with subcostal retractions. The physical examination disclosed no other abnormalities. A chest radiograph revealed mild ground-glass opacity in both the lungs. The infant needed assisted mechanical ventilation.
Blood tests performed 1 hour after delivery showed hemoglobin concentration of 11.9 g/dL and a platelet count of 76,000/╬╝L. Additional blood tests revealed a prothrombin time (PT) of 12.1 seconds (normal 10.6 to 16.2), activated partial thromboplastin time of 60.6 seconds (normal 27.5 to 79.4), fibrinogen levels of 72.4 mg/dL (normal 150 to 373), and elevated D-dimer levels >3,200 ng/mL (normal <500). Hematologic laboratory values throughout the hospital course are shown in Figure 1.
Despite repeated transfusions of packed red blood cells, platelets, fresh frozen plasma, and cryoprecipitate, his clinical condition and coagulopathy gradually worsened.
Renal ultrasonography was performed on the 6th hospital day to determine the origin of the coagulopathy. The renal ultrasonography revealed an echogenic mass measuring >3 cm in the abdominal cavity and diffuse increased echogenicity of the right kidney with hydronephrosis (Figure 2). Brain ultrasonography performed on the 10th hospital day showed no abnormality.
A magnetic resonance imaging (MRI) scan of the abdomen showed an ill-marginated, infiltrative mass like lesion in the right anteromedial and posteromedial perirenal space that was hypointense with mild enhancement on T1- and T2-weighted images and right hydronephrosis with an intrarenal hematoma (Figure 2).
Because the MRI findings were inconclusive, he underwent exploratory laparotomy on the 12th hospital day. Large vascular tumors adherent to other visceral organs (including the colonic mesentery, kidney, and adrenal gland) were observed but could not be resected due to a high risk of uncontrolled bleeding.
The presumptive diagnosis of KHE with KMP was made due to the infiltrative appearance of the mass, and treatment with methylprednisolone (1.6 mg/kg daily) was initiated on the 15th hospital day.
The right hydronephrosis was aggravated due to the mass surrounding the right renal hilum, and the renal function progressively worsened with decreased urine output on the 13th hospital day and his serum creatinine levels elevating to 1.09 mg/dL on the 14th hospital day. On the 16th hospital day, a percutaneous nephrostomy was placed due to deterioration of obstructive nephropathy.
Because the coagulopathy did not improve and the patient's condition worsened despite treatment with methylprednisolone for 2 days, vincristine (0.05 mg/kg/dose) was added and administered weekly from the 17th hospital day. The coagulation profile showed gradual improvement after vincristine therapy. Eventually, the fibrinogen concentration and the platelet count was normalized on the 48th and 54th hospital day, respectively. Intravenous methylprednisolone was switched to oral prednisolone from the 57th hospital day. On the 60th hospital day, the nephrostomy was removed. The patient was discharged on the 73rd hospital day. The prednisolone dose was slowly tapered starting on the 60th hospital day and stopped at 9 weeks after the start of prednisolone treatment. Furthermore, after seven cycles of weekly vincristine, we extended the dosing interval for vincristine from once a week to once every 2 weeks at the same dose. The patient continued vincristine treatment every 2 weeks as an outpatient treatment and it was suspended after 8 weeks. Taken together, corticosteroids and 12 cycles of vincristine were administered for a total of 16 weeks.
Currently the patient has not received any treatment, and there has been no recurrence with a complete regression of the tumor at the 39-month follow-up (Figure 3). Although his weight and height are between the 5th and 10th percentiles for his age, he is currently healthy and neurologically normal.
We report a neonatal case of visceral KHE with KMP that responded to treatment with systemic corticosteroids and vincristine without side effects. KMP is a rare thrombocytopenic consumption coagulopathy associated with an enlarging vascular tumor, hemangioma, or vascular malformation, originally described in 1940 [4].
Gilon et al. [5]. described that the platelet concentration was higher in the hemangioma vessel of patients with multiple and extended hemangiomata than in the peripheral blood. Brizel and Raccuglia [6] showed increased radioactivity over the hemangioma after an infusion of 51 Cr-tagged platelets due to platelet sequestration in the tumor. Platelet trapping in the vascular lumen of the tumor was also demonstrated by an immunohistochemical technique using an anti-CD61 antibody [7]. This platelet trapping activates an intravascular coagulation and results in the depletion of clotting factors [8].
A retroperitoneal hemangioma is often huge with a high mortality rate [8]. Our patientŌĆÖs overall clinical condition gradually deteriorated despite receiving intensive clinical supportive measures, including platelets, fresh frozen plasma, and packed erythrocyte infusions daily; he eventually survived after receiving vincristine in combination with steroids.
Curative surgical excision is the definitive treatment for KHE, but it may not be possible depending on the location of the tumor [9]. Cases in which the lesions were resectable and treated with surgery have been reported [9]. However, KHEs usually show an infiltrative nature and have no clear boundaries for resection [10]. It is also problematic that the tumor may recur if the lesion remains after surgery [11]. Although large vascular tumors adhering to other visceral organs were found in our case, they were not resected due to the risk of uncontrolled, lethal bleeding.
Drucker et al. [12]. reported a successful treatment of a KHE located on the right leg in a newborn with a combination of corticosteroids and vincristine. The case described in that report presented with cutaneous KHE. However, we successfully treated the visceral form of KHE known to be lethal using those two drugs. Consensus-based medical treatments with corticosteroids and/or vincristine were recommended by a multidisciplinary expert panel in 2013 [10]. However, other treatment regimens have been attempted for KHE with KMP because the effects of the proposed guidelines are limited. Cases when either steroid or vincristine treatment was used in combination with other drugs have been reported. Hauer et al. [13]. reported a case of a 6-month-old girl who suffered from a KHE of the chest wall with KMP and was in remission after six cycles of the applied four-drug regimen (vincristine combined with cyclophosphamide, actinomycin D, and methotrexate). Barabash-Neila et al. [14]. reported a case of a 24- day-old boy presenting with a progressively enlarging tumor involving the left cheek area, thrombocytopenia, hypofibrinogenemia, and elevated D-dimer levels. He was diagnosed with KHE with KMP based on clinical and laboratory findings and successfully treated with systemic corticosteroids, ticlopidine, aspirin, and vincristine. Administering corticosteroid alone has its limitations owing to refractory cases and recurrence [12]. Furthermore, prolonged corticosteroid therapy can cause side effects such as immunosuppression and glucose intolerance [15]. By administering vincristine and fewer steroids, side effects can be reduced. Lopez et al. [16]. also reported a case of treatment using vinristine and ticlopidine. Mizutani et al. [17]. presented a case of an otherwise healthy newborn boy born with a large mass on the right chest who was administered systemic prednisolone in an attempt to treat thrombocytopenia and coagulopathy. The tumor did not regress despite hematologic improvement, but the tumor size decreased after adding oral propranolol to prednisolone therapy [17]. Although the effects of propranolol in the treatment of infantile hemangiomas have been demonstrated, the effects of propranolol monotherapy on KMP are limited [17]. Most recently, there was a case report of successful treatment using prednisolone, vincristine, and sirolimus [18]. Percutaneous transarterial embolization could be another therapeutic option. Garcia-Monaco et al. [19]. introduced cases of successful treatment of KHE with embolization and vincristine in two newborns.
Interferon-╬▒ (IFN-╬▒), which inhibits angiogenesis, can be considered as a treatment option [20]. Several cases of KHE effectively treated with IFN-╬▒ have been reported [20]. However, it should be used cautiously in patients under 1 year of age due to the risk of spastic diplegia [10].
Low-dose radiotherapy can be administered either alone or in combination with other treatment modalities, even though this treatment is sometimes avoided because of its known effects on growth and secondary malignancies [8].
In our case, although treatment using a systemic corticosteroid was attempted first, there was no apparent therapeutic response. After introducing vincristine, the clinical and laboratory findings gradually improved.
In conclusion, our patient showed a dramatic improvement in symptoms and laboratory parameters after administering a combination therapy involving prednisolone and vincristine. We can consider combination therapy of systemic corticosteroids and vincristine in life-threatening KHE as a first-line treatment, and other drugs or modalities can be added if needed.
ARTICLE INFORMATION
Figure┬Ā1.
Hematologic laboratory values during the hospital course. D-dimer levels >3,200 ng/mL are indicated as 32├Ś102 ng/mL in the graph.

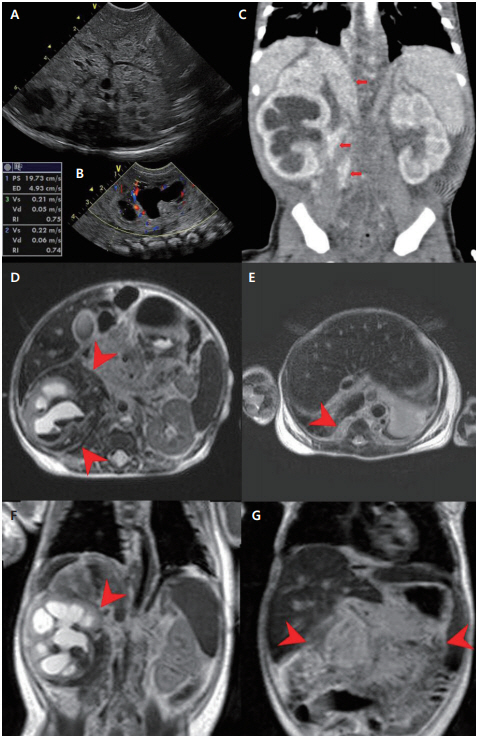
Figure┬Ā2.
Imaging studies of the patient. (A) Renal ultrasonography performed on the 6th day of life showing diffusely echogenic soft tissue surrounding the inferior vena cava, aorta, and its branches. (B) Renal ultrasonography performed on the 6th day of life showing diffusely increased parenchymal echogenicity of the right kidney with hydronephrosis. (C) Abdominopelvic computed tomography performed on the 7th day of life showing diffuse, ill-marginated enhancing lesion surrounding the right renal hilum and right inferomedial aspects of the perirenal space (indicated by arrows). (D) Abdominal magnetic resonance imaging (MRI) scan showing diffuse, ill-marginated infiltrative mass like lesion on the right anteromedial and posteromedial aspects of the perirenal space. (E) Abdominal MRI scan showing asymmetric thickening of right crura. (F) Abdominal MRI scan showing right hydronephrosis and hemorrhage/hematoma inside the right kidney. (G) Abdominal MRI scan showing the mesentery with diffuse high signal intensity on a T1-weighted image (indicated by arrowheads).
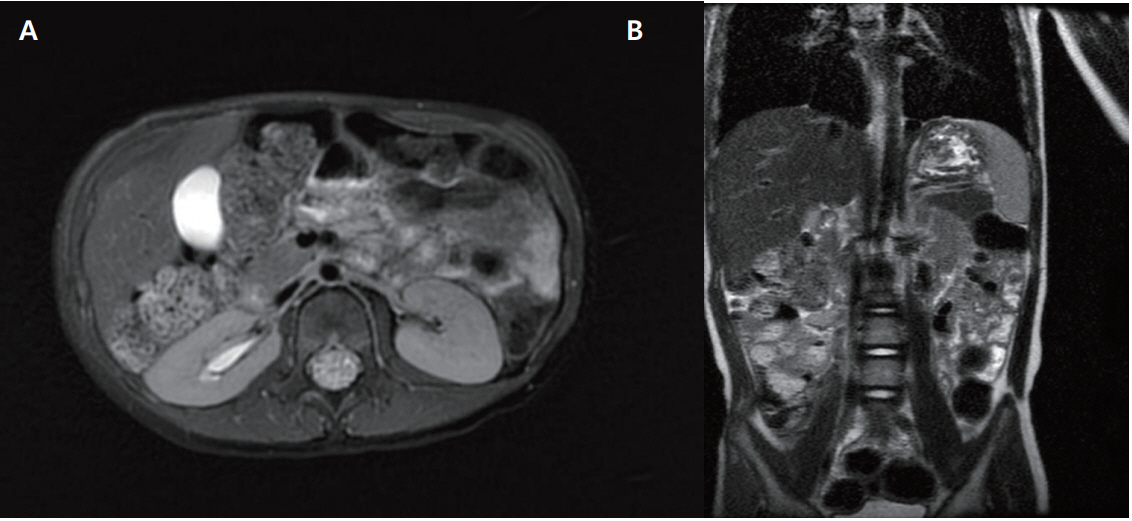
Figure┬Ā3.
Follow-up magnetic resonance imaging performed at 39 months of age. (A, B) Unremarkable finding in the right perirenal space and the upper abdomen except for mild right hydronephrosis.
REFERENCES
1. Fletcher CDM, World Health Organization. WHO classification of tumours of soft tissue and bone. 4th ed. Lyon:International Agency for Research on Cancer, 2013, pp 110ŌĆō1.
2. Fernandez Y, Bernabeu-Wittel M, Garcia-Morillo JS. Kaposiform hemangioendothelioma. Eur J Intern Med 2009;20:106ŌĆō13.


3. Nakaya T, Morita K, Kurata A, Ushiku T, Igarashi T, Kuroda M, et al. Multifocal kaposiform hemangioendothelioma in multiple visceral organs: an autopsy of 9-day-old female baby. Hum Pathol 2014;45:1773ŌĆō7.


4. Kasabach HH, Merritt KK. Capillary hemangioma with extensive purpura: report of a case. Am J Dis Child 1940;59:1063ŌĆō70.

5. Gilon E, Ramot B, Sheba C. Multiple hemangiomata associated with thrombocytopenia: remarks on the pathogenesis of the thrombocytopenia in this syndrome. Blood 1959;14:74ŌĆō9.



6. Brizel HE, Raccuglia G. Giant hemangioma with thrombo cytopenia. Radioisotopic demonstration of platelet sequestra tion. Blood 1965;26:751ŌĆō64.



7. Seo SK, Suh JC, Na GY, Kim IS, Sohn KR. Kasabach-Merritt syndrome: identification of platelet trapping in a tufted angioma by immunohistochemistry technique using monoclonal anti body to CD61. Pediatr Dermatol 1999;16:392ŌĆō4.


8. Hall GW. Kasabach-Merritt syndrome: pathogenesis and mana gement. Br J Haematol 2001;112:851ŌĆō62.


9. Pascal S, Bettex Q, Andre N, Petit P, Casanova D, Degardin N. Successful surgical management of congenital KasabachMerritt syndrome. Pediatr Int 2017;59:89ŌĆō92.


10. Drolet BA, Trenor CC 3rd, Brandao LR, Chiu YE, Chun RH, Dasgupta R, et al. Consensus-derived practice standards plan for complicated Kaposiform hemangioendothelioma. J Pediatr 2013;163:285ŌĆō91.


11. Kim MG, Choi YS, Park SJ, Chong SM. Kaposiform hemangioendothelioma of the breast in an adult female. Clin Breast Can cer 2011;11:135ŌĆō7.

12. Drucker AM, Pope E, Mahant S, Weinstein M. Vincristine and corticosteroids as first-line treatment of Kasabach-Merritt syndrome in kaposiform hemangioendothelioma. J Cutan Med Surg 2009;13:155ŌĆō9.


13. Hauer J, Graubner U, Konstantopoulos N, Schmidt S, Pfluger T, Schmid I. Effective treatment of kaposiform hemangioendotheliomas associated with Kasabach-Merritt phenomenon using four-drug regimen. Pediatr Blood Cancer 2007;49:852ŌĆō4.


14. Barabash-Neila R, Garcia-Rodriguez E, Bernabeu-Wittel J, Bueno-Rodriguez I, Ramirez-Villar G, Lopez-Gutierrez JC. Kaposiform hemangioendothelioma with Kasabach-Merritt phenomenon: successful treatment with vincristine and ticlopidine. Indian J Pediatr 2012;79:1386ŌĆō7.



15. Greinwald JH Jr, Burke DK, Bonthius DJ, Bauman NM, Smith RJ. An update on the treatment of hemangiomas in children with interferon alfa-2a. Arch Otolaryngol Head Neck Surg 1999;125:21ŌĆō7.


16. Lopez V, Marti N, Pereda C, Martin JM, Ramon D, Mayordomo E, et al. Successful management of Kaposiform hemangio endothelioma with Kasabach-Merritt phenomenon using vincristine and ticlopidine. Pediatr Dermatol 2009;26:365ŌĆō6.


17. Mizutani K, Umaoka A, Tsuda K, Kakeda M, Habe K, Yamanaka K, et al. Successful combination therapy of propranolol and prednisolone for a case with congenital Kasabach-Merritt syndrome. J Dermatol 2017;44:1389ŌĆō91.


18. Cashell J, Smink GM, Helm K, Xavier F. Kaposiform hemangioendothelioma with Kasabach-Merritt phenomenon in an infant: Successful treatment with prednisolone, vincristine, and addition of sirolimus. Pediatr Blood Cancer 2018;65:e27305.


-
METRICS

-
- 1 Crossref
- 5,068 View
- 91 Download
- Related article in NM






